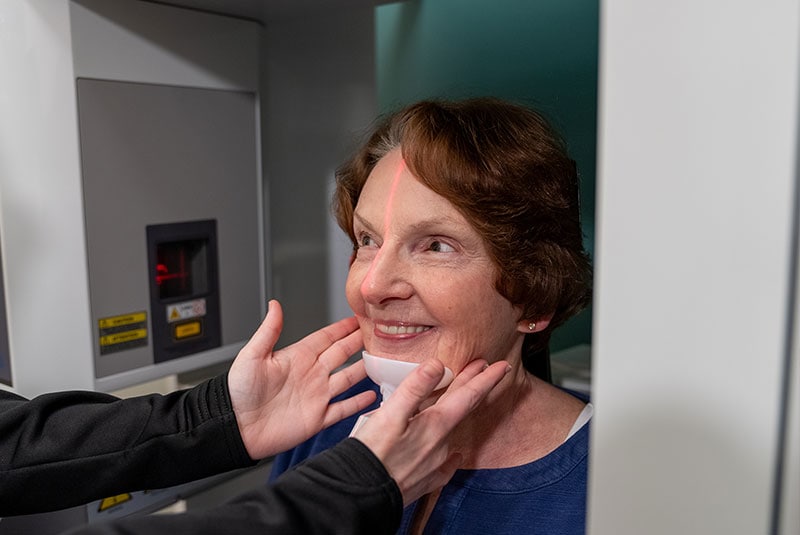
Major & Minor Bone Grafting
Missing teeth over a period of time can cause your jaw bone to atrophy, or resorb. This often results in poor quality and quantity of bone suitable for the placement of dental implants as well as long-term shifting of remaining teeth and changes to facial structure. Bone grafting makes implant restorations a reality for these patients who would otherwise not be candidates for implants.
Fortunately, today we have the ability to grow bone where it is needed. This not only gives us the opportunity to place implants of proper length and width, but it also gives us a chance to restore functionality and aesthetic appearance.
Major Bone Grafting
Bone grafting can repair implant sites with inadequate bone structure due to previous extractions, gum disease, or injuries. The bone is either obtained from a tissue bank or your own bone is taken from the jaw, hip, or tibia (below the knee). Sinus bone grafts are also performed to replace bone in the posterior upper jaw. In addition, special membranes may be utilized to protect the bone graft, as well as encourage bone regeneration. This is called guided bone regeneration, or guided tissue regeneration.
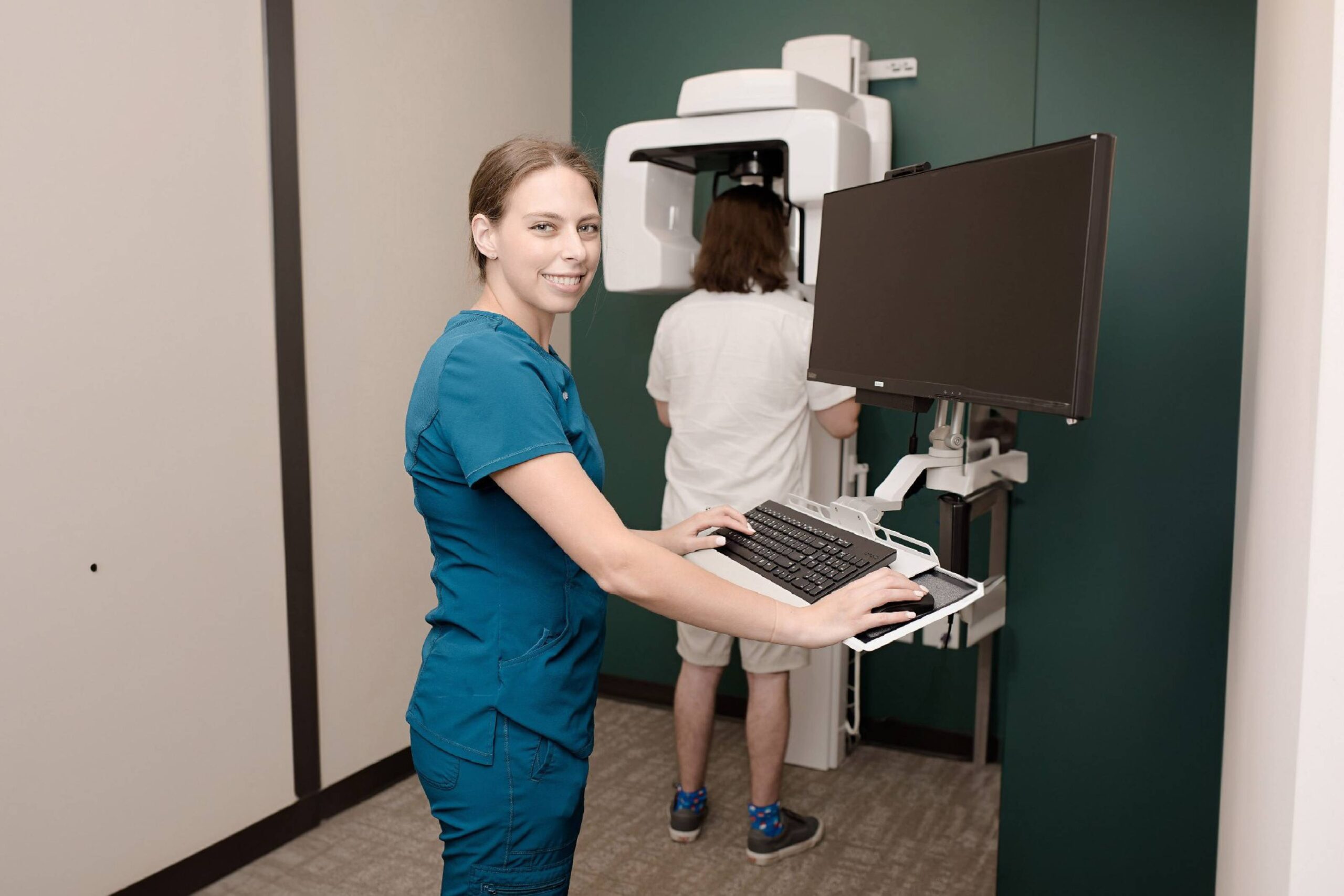
Major bone grafts are typically performed to repair defects in the jaws. These defects may arise as a result of traumatic injuries, tumor surgery, or congenital defects. Large defects are repaired using the patient’s own bone. This bone is harvested from a number of different areas depending on the size needed. The skull (cranium), hip (iliac crest), and lateral knee (tibia) are common donor sites. These procedures are routinely performed in an operating room and require a hospital stay.
The Importance of Teeth for Jaw Bone Health
When one or more teeth are missing it can lead to bone loss at the site of the gap. This loss of jaw bone can develop into additional problems, both with your appearance and your overall health. You may experience pain, problems with your remaining teeth, altered facial appearance, and eventually even the inability to speak and/or eat normally.
In the same way that muscles are maintained through exercise, bone tissue is maintained by use. Natural teeth are embedded in the jaw bone and stimulate the jaw bone through activities such as chewing and biting. When teeth are missing, the alveolar bone, or the portion of the jaw bone that anchors the teeth into the mouth, no longer receives the necessary stimulation it needs and begins to break down or resorb. The body no longer uses or “needs” the jaw bone, so it deteriorates.
Potential Consequences of Tooth & Jaw Bone Loss
- Problems with remaining teeth, including misalignment, drifting, loosening, and loss
- Collapsed facial profile
- Limited lip support
- Skin wrinkling around the mouth
- Distortion of other facial features
- Jaw (TMJ or temporomandibular joint) pain, facial pain, and headaches
- Difficulty speaking and communicating
- Inadequate nutrition as a result of the inability to chew properly and painlessly
- Sinus expansion
Reasons for Jaw Bone Loss & Deterioration
The following are the most common causes of jaw bone deterioration and loss that may require a bone grafting procedure:
Tooth Extractions
When an adult tooth is removed and not replaced, jaw bone deterioration may occur. Natural teeth are embedded in the jaw bone and stimulate the jaw bone through activities such as chewing and biting. When teeth are missing, the alveolar bone, or the portion of the jaw bone that anchors the teeth in the mouth, no longer receives the necessary stimulation and begins to break down, or resorb. The body no longer uses or “needs” the jaw bone, so it deteriorates and goes away.
The rate at which the bone deteriorates, as well as the amount of bone loss that occurs, varies greatly among individuals. However, most loss occurs within the first eighteen months following the extraction and will continue gradually throughout your life.
Periodontal Disease
Periodontal diseases are ongoing infections of the gums that gradually destroy the support of your natural teeth. Periodontal disease affects one or more of the periodontal tissues: alveolar bone, periodontal ligament, cementum, or gingiva. While there are many diseases that affect the tooth-supporting structures, plaque-induced inflammatory lesions make up the majority of periodontal issues and are divided into two categories: gingivitis and periodontitis. While gingivitis, the less serious of the diseases, may never progress into periodontitis, it always precedes periodontitis.
Dental plaque is the primary cause of gingivitis in genetically susceptible individuals. Plaque is a sticky colorless film, composed primarily of food particles and various types of bacteria, that adheres to your teeth at and below the gum line. Plaque constantly forms on your teeth, even minutes after cleaning. Bacteria found in plaque produce toxins, or poisons, that irritate the gums. Gums may become inflamed, red, swollen, and bleed easily. If this irritation is prolonged, the gums will separate from the teeth causing pockets (spaces) to form. If daily brushing and flossing are neglected, plaque can harden into a rough, porous substance known as calculus (or tartar). This can occur both above and below the gum line.
Periodontitis is affected by bacteria that adhere to the tooth’s surface, along with an overly aggressive immune response to these bacteria. If gingivitis progresses into periodontitis, the supporting gum tissue and bone that hold teeth in place deteriorates. The progressive loss of this bone, the alveolar, can lead to the loosening and subsequent loss of teeth.
Dentures/Bridgework
Unanchored dentures are placed on top of the gum line, but they do not provide any direct stimulation to the underlying alveolar bone. Over time the lack of stimulation causes the bone to resorb and deteriorate. Because this type of denture relies on the bone to hold them in place, people often experience loosening of their dentures and problems eating and speaking. Eventually, bone loss may become so severe that dentures cannot be held in place with strong adhesives, and a new set of dentures may be required. Proper denture care, repair, and refitting are essential to maintaining oral health.
Some dentures are supported by anchors, which help adequately stimulate, and therefore preserve bone.
With bridgework, the teeth on either side of the appliance provide sufficient stimulation to the bone, but the portion of the bridge that spans the gap where the teeth are missing receives no direct stimulation. Bone loss can occur in this area.
By completing a bone graft procedure, your doctor is now able to restore bone function and growth, thereby halting the effects of poor denture care.
Facial Trauma
When a tooth is knocked out or broken to the extent that no biting surface is left below the gum line, bone stimulation stops, which results in jaw bone loss. Some common forms of tooth and jaw trauma include: teeth knocked out from injury or accident, jaw fractures, or teeth with a history of trauma that may die and lead to bone loss years after the initial trauma.
A bone grafting procedure would be necessary to reverse the effects of bone deterioration, restoring function and promoting new bone growth in traumatized areas.
Misalignment
Misalignment issues can create a situation in the mouth where some teeth no longer have an opposing tooth structure. The unopposed tooth can over-erupt, causing deterioration of the underlying bone.
Issues such as TMJ problems, normal wear-and-tear, and lack of treatment can also create abnormal physical forces that interfere with the teeth’s ability to grind and chew properly. Over time, bone deterioration can occur where the bone is losing stimulation.
Osteomyelitis
Osteomyelitis is a type of bacterial infection in the bone and bone marrow of the jaw. This infection leads to inflammation, which can cause a reduction of blood supply to the bone. Treatment for osteomyelitis generally requires antibiotics and the removal of the affected bone. A bone graft procedure may be required to restore bone function and growth lost during removal.
Tumors
Benign facial tumors, though generally non-threatening, may grow large and require the removal of a portion of the jaw. Malignant mouth tumors almost always spread into the jaw, requiring the removal of the affected section of the jaw. In both cases, reconstructive bone grafting is usually required to help restore normal function to the jaw. Grafting in patients with malignant tumors may be more challenging because treatment of the cancerous tumor generally requires the removal of the surrounding soft tissues as well.
Developmental Deformities
Some conditions or syndromes are characterized by missing portions of the teeth, facial bones, jaw, or skull. Your doctor may be able to perform a bone graft procedure to restore bone function and growth where it may be absent.
Sinus Deficiencies
When molars are removed from the upper jaw, air pressure from the air cavity in the maxilla (maxillary sinus) causes resorption of the bone that formerly helped keep the teeth in place. As a result, the sinuses become enlarged, a condition called hyperpneumatized sinus.
This condition usually develops over several years and may result in insufficient bone from the placement of dental implants. Your doctor can perform a procedure called a “sinus lift” that can treat enlarged sinuses.
About Bone Grafting
What is Bone Grafting?
Over a period of time, the jaw bone associated with missing teeth atrophies and is reabsorbed. This often leaves a condition in which there is poor quality and quantity of bone suitable for the placement of dental implants. In these situations, most patients are not candidates for the placement of dental implants.
With bone grafting, we now have the opportunity to not only replace bone where it is missing, but we also have the ability to promote new bone growth in that location. This not only gives us the opportunity to place implants of proper length and width, it also gives us a chance to restore functionality and aesthetic appearance.
Types of Bone Grafts
Autogenous Bone Grafts
Autogenous bone grafts, also known as autografts, are made from your own bone, taken from somewhere else in the body. The bone is typically harvested from the chin, jaw, lower leg bone, hip, or skull. Autogenous bone grafts are advantageous in that the graft material is your own live bone, meaning it contains living cellular elements that enhance bone growth, also eliminating the risk of your body rejecting the graft material since it comes from you.
However, one downside to the autograft is that it requires a second procedure to harvest bone from elsewhere in the body. Depending on your condition, a second procedure may not be recommended.
Allogenic Bone
Allogenic bone, or allograft, is dead bone harvested from a cadaver, then processed using a freeze-dry method to extract the water via a vacuum. Unlike autogenous bone, allogenic bone cannot produce new bone on it’s own. Rather, it serves as a framework, or scaffold, over which bone from the surrounding bony walls can grow to fill the defect or void.
Xenogenic Bone
Xenogenic bone is derived from the non-living bone of another species, usually a cow. The bone is processed at very high temperatures to avoid the potential for immune rejection and contamination. Like allogenic grafts, xenogenic grafts serve as a framework for bone from the surrounding area to grow and fill the void.
Both allogenic and xenogenic bone grafting have the advantage of not requiring a second procedure to harvest your own bone, as with autografts. However, because these options lack autograft’s bone-forming properties, bone regeneration may take longer than with autografts, and have a less predictable outcome.
Bone Graft Alternatives
As a substitute to using real bone, many synthetic materials are available as safe and proven alternatives, including:
Demineralized Bone Matrix (DBM)/Demineralized Freeze-Dried Bone Allograft (DFDBA)
This product is processed allograft bone, containing collagen, proteins, and growth factors that are extracted from the allograft bone. It is available in the form of powder, putty, chips, or as a gel that can be injected through a syringe.
Graft Composites
Graft composites consist of other bone graft materials and growth factors to achieve the benefits of a variety of substances. Some combinations may include a collagen/ceramic composite, which closely resembles the composition of natural bone, DBM combined with bone marrow cells, which aid in the growth of new bone, or a collagen/ceramic/autograft composite.
Bone Morphogenetic Proteins
Bone morphogenetic proteins (BMPs) are proteins naturally produced in the body that promote and regulate bone formation and healing.
Synthetic materials also have the advantage of not requiring a second procedure to harvest bone, reducing risk and pain. Each bone grafting option has its own risks and benefits. One of our doctors will determine which type of bone graft material is best suited to your particular needs.
Socket Preservation Procedure
Preserving Your Jaw Bone After Extractions
Removal of teeth is sometimes necessary because of pain, infection, bone loss, or due to a fracture in the tooth. The bone that holds the tooth in place (the socket) is often damaged by disease and/or infection, resulting in a deformity of the jaw after the tooth is extracted. In addition, when teeth are extracted the surrounding bone and gums can shrink and recede very quickly, resulting in unsightly defects and a collapse of the lips and cheeks.
These jaw defects can create major problems in performing restorative dentistry whether your treatment involves dental implants, bridges, or dentures. Jaw deformities from tooth removal can be prevented and repaired by a procedure called socket preservation. Socket preservation can greatly improve your smile’s appearance and increase your chances for successful dental implants.
Several techniques can be used to preserve the bone and minimize bone loss after an extraction. In one common method, the tooth is removed and the socket is filled with bone or bone substitute. It is then covered with gum, artificial membrane, or tissue, which encourages your body’s natural ability to repair the socket. With this method, the socket heals, eliminating shrinkage and collapse of the surrounding gum and facial tissues. The newly formed bone in the socket also provides a foundation for an implant to replace the tooth. If your dentist has recommended tooth removal, be sure to ask if socket preservation is necessary. This is particularly important if you are planning on replacing the front teeth.
What is a Ridge Augmentation?
A ridge augmentation is a common dental procedure often performed following a tooth extraction. This procedure helps recreate the natural contour of the gums and jaw that may have been lost due to bone loss from a tooth extraction, or for another reason.
The alveolar ridge of the jaw is the bone that surrounds the roots of teeth. When a tooth is removed an empty socket is left in the alveolar ridge bone. Usually, this empty socket will heal on its own, filling with bone and tissue. Sometimes when a tooth is removed the bone surrounding the socket breaks and is unable to heal on its own. The previous height and width of the socket will continue to deteriorate.
Rebuilding the original height and width of the alveolar ridge is not always medically necessary, but may be required for dental implant placement or for aesthetic purposes. Dental implants require bone to support their structure and a ridge augmentation can help rebuild this bone to accommodate the implant.
How is a Ridge Augmentation Accomplished?
A ridge augmentation is accomplished by placing bone graft material in the tooth socket. It is often done immediately after the tooth is removed to avoid the need for a second procedure later. Next, the gum tissue is placed over the socket and secured with sutures. Your doctor may choose to use a space-maintaining product over the top of the graft to facilitate new bone growth. Once the socket has healed, the alveolar ridge can be prepared for dental implant placement.
A ridge augmentation procedure is typically performed in our office under local anesthesia or IV sedation, depending on the complexity of the procedure. Some patients may also request sedative medication.
What is a Sinus Lift?
The maxillary sinuses are behind your cheeks and on top of the upper teeth. These sinuses are empty, air-filled spaces. Some of the roots of the natural upper teeth extend up into the maxillary sinuses. When these upper teeth are removed there is often just a thin wall of bone separating the maxillary sinus and the mouth. Dental implants need bone to hold them in place. When the sinus wall is very thin, it is impossible to place dental implants in this bone.
The key to a successful and long-lasting dental implant is the quality and quantity of jaw bone to which the implant will be attached. If bone loss has occurred due to injury or periodontal disease, a sinus augmentation can raise the sinus floor and allow for new bone formation. A sinus lift is one of the most common bone grafting procedures for patients with bone loss in the upper jaw. The procedure seeks to grow bone in the floor of the maxillary sinus above the bony ridge of the gum line that anchors the teeth in the upper jaw. This enables dental implants to be placed and secured in the new bone growth.
Do I Need a Sinus Lift?
A sinus lift may be necessary if you:
- Are missing more than one tooth in the back of your jaw
- Are missing a significant amount of bone in the back of your jaw
- Are missing teeth due to a birth defect or condition
- Are missing most of the maxillary teeth and require support for dental implants
How is a Sinus Lift Accomplished?
Most commonly, a small incision is made on the premolar or molar region to expose the jaw bone. A small opening is cut into the bone, and the membrane lining the sinus is pushed upward. The underlying space is filled with bone grafting material, either from your own body or from other sources. Sometimes, synthetic materials that imitate bone formation are used. After the bone is implanted, the incision is sutured and the healing process begins. After several months of healing, the bone becomes part of the patient’s jaw, and dental implants can be inserted and stabilized in the newly formed sinus bone.
If enough bone between the upper jaw ridge and the bottom of the sinus is available to sufficiently stabilize the implant, sinus augmentations, and implant placement can sometimes be performed as a single procedure. If not enough bone is available, the sinus augmentation will have to be performed first, then the graft will have to mature for up to several months, depending upon the type of graft material used. Once the graft has matured, the implants can be placed.
The sinus graft makes it possible for many patients to have dental implants that previously had no other option besides wearing loose dentures.
A sinus augmentation is generally performed at Dr. Collins, Dr. Haws’, and Dr. Hull‘s office, under local anesthesia. Some patients may request oral or intravenous sedative medication as well.
Nerve Repositioning
The inferior alveolar nerve, which gives feeling to the lower lip and chin, may need to be moved in order to make room for the placement of dental implants in the lower jaw. A nerve repositioning procedure is limited to the lower jaw and may be indicated when teeth are missing in the area of the two back molars and/or second premolars. This procedure is considered a very aggressive approach since there is almost always some postoperative numbness of the lower lip and jaw area, which typically dissipates very slowly, but may be permanent. Usually other, less aggressive options are considered first (placement of blade implants, etc).
Typically, we remove an outer section of the cheek on the side of the lower jaw bone in order to expose the nerve and vessel canal. We then isolate the nerve and vessel bundle in that area and slightly pull it out to the side. We then place the implants while tracking the neuro-vascular bundle. Then the bundle is released and placed back over the implants. The surgical access is refilled with bone graft material of the surgeon’s choice and the area is closed.
These procedures may be performed separately or together depending upon the individual’s condition. As stated earlier, there are several areas of the body that are suitable for attaining bone grafts. In the maxillofacial region, bone grafts can be taken from inside the mouth, in the area of the chin or third molar region, or in the upper jaw behind the last tooth. In more extensive situations a greater quantity of bone can be attained from the hip or the outer aspect of the tibia at the knee. When we use the patient’s own bone for repairs or additions, we generally get the best results.
In many cases, we can use allograft material to implement bone grafting for dental implants. This bone is prepared from cadavers and is used to get the patient’s own bone to grow into the repair site. It is quite effective and very safe. Synthetic materials can also be used to stimulate bone formation. We even use factors from your own blood to accelerate and promote bone formation in graft areas.
These surgeries are performed in the out-of-office surgical suite under IV sedation or general anesthesia. After discharge, bed rest is recommended for one day, as well as limited physical activity for one week.